
The skin barrier. Often misunderstood or simply forgotten but absolutely essential to skin health. and today’s deep dive is ALL about it.
Yes, we’ve briefly touched on the skin barrier in other blog posts and will also be continuing to explore other facial anatomy soon! But in chatting with many of you in our Facebook community, I think a dedicated deep dive on the skin barrier is needed. It serves such an important function and is also involved in so many common skin concerns from acne to dry skin.
Before we get started, I want to add that we use correct medical terms around here. I see “moisture barrier” tossed around by many influencers but this isn’t an actual term and I encourage everyone to stick to skin barrier if “stratum corneum barrier” or “epidermal barrier” is too wordy.
Some links and codes are affiliate. They add no cost to you, the reader, but help support the author and her content. Some images in this post are also from published scientific journals, please click the image to see the original source and for additional information on that topic.
Skin Barrier Anatomy
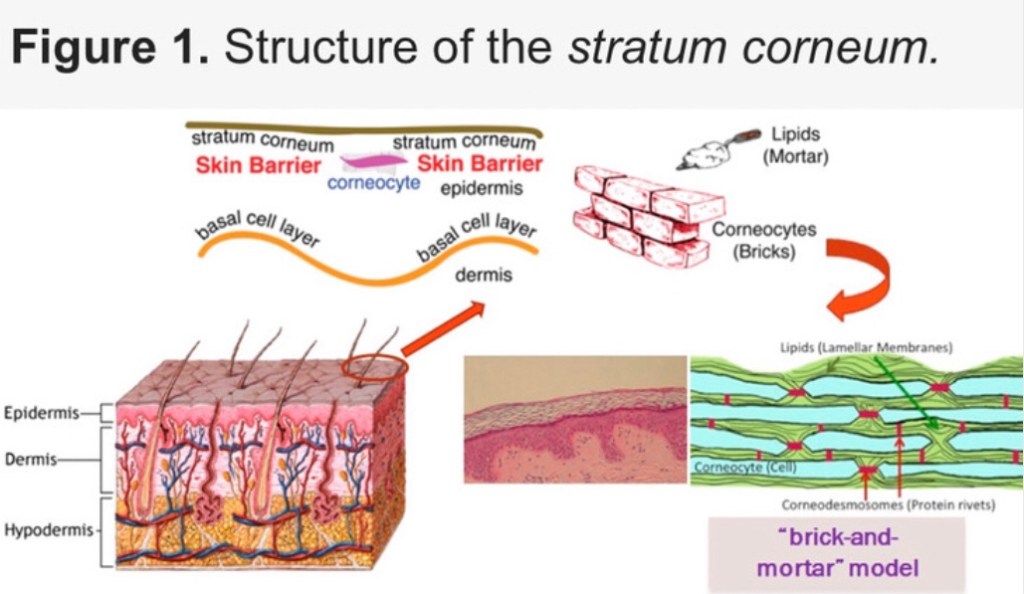
Layers of the Epidermis
In order to have a better understanding of the cells that make up the stratum corneum, we need to know that cell division occurs at the deepest layer of the epidermis – the stratum basale.
Consisting of a single layer of basal cells (the stem cells of the epidermis essentially), this part of the epidermis is responsible for all epidermal cell proliferation. These cells divide into 2 daughter cells and each new cell layer pushes the next row of cells outward from the stratum basale to the stratum spinosum and then upward through the other epidermal layers all the way up to the stratum corneum finally. You may have heard of this process referred to as cell renewal or cell turnover which slows down as we get older.
See the image below to see the layers of the epidermis (the top layer of skin that sits on top of the dermis). Please note that the stratum lucidum is only present in the thick skin found in areas like the palms of our hands.
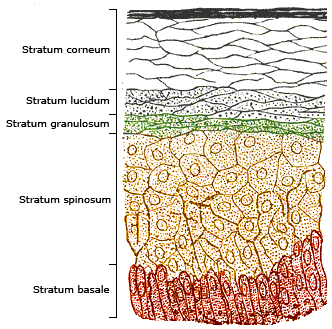
The Stratum Corneum
90% of epidermal cells are keratinocytes, responsible for producing the protein keratin. By the time they reach the stratum corneum, they’re technically dead and filled with keratin. These cells serve many important functions in the epidermis but their main function relates to the skin barrier. In the stratum granulosum, keratinocytes will release the lipids that will then fill the intracellular spaces in the skin barrier – called the lipid matrix. The keratinocytes then differentiate into corneocytes, the long flat cells that also make up the stratum corneum barrier with the lipids in between.
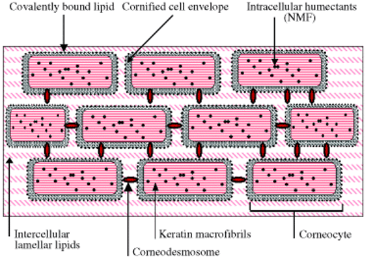
In the medical field, the “brick and mortar skin model” is a common analogy used to describe this barrier. The bricks are the corneocytes while the mortar is the lipid matrix. See the image below for a visual.
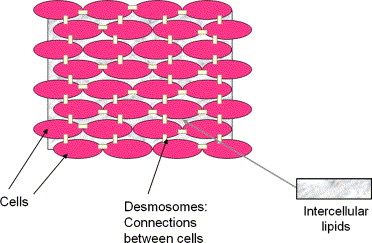
The corneocytes contain our Natural Moisturizing Factor (NMF) – aka our skin’s natural humectants – while the lipids are made up of mainly ceramides, cholesterol, and fatty acids. In the next section on skin barrier function, we’ll cover how these components work together to attract and retain moisture while keeping pathogens and environmental factors out.
Okay, so we covered the layers of the epidermis and the stratum corneum in particular. That about covers the anatomy portion, right? Not quite. In discussing the structure of the skin barrier, it’s also critical to discuss the pH gradient and the skin microbiome.
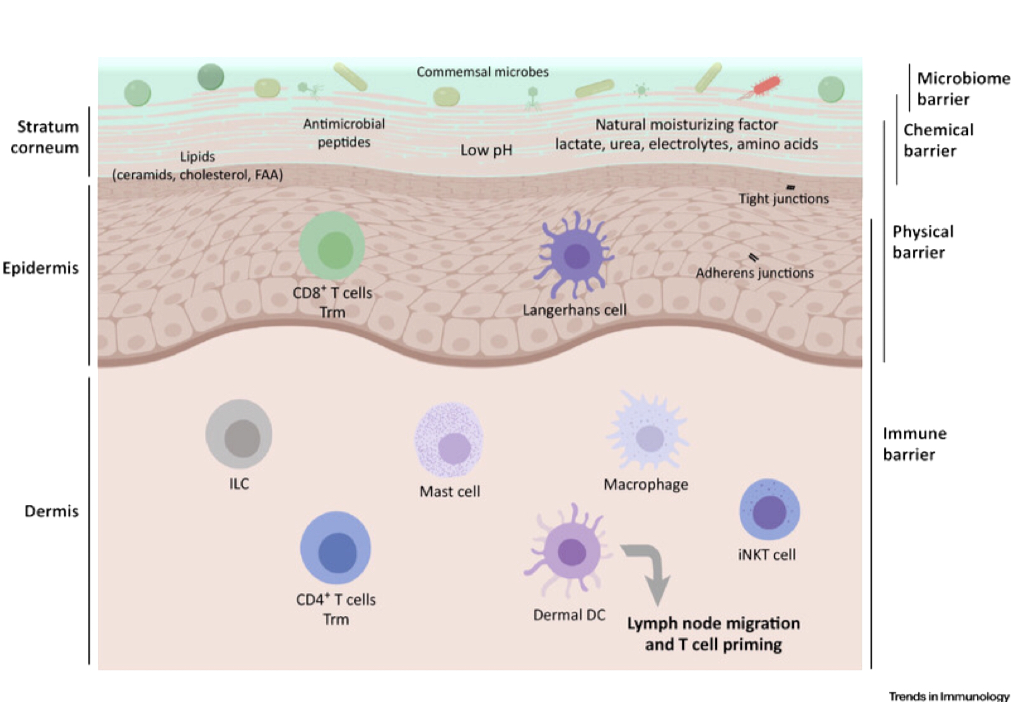
The skin has a diverse microbiota often referred to as the skin flora and is made up of many different bacteria, viruses, and other microorganisms like yeast. The skin surface is an inhospitable environment thanks to the acidic surface pH and lack of nutrients so these microorganisms have adapted to these harsh conditions. The skin flora is actually critical to overall skin health and as we will cover further along, an increase in pH can dispel these beneficial microorganisms and means less competition and a friendlier environment to pathogens.
Looking at the image above, you can see that the skin barrier is actually compromised of multiple barriers in truth – from the microbial to the chemical and physical. The surface of the skin is acidic, with healthy skin often measuring below pH 5. But as you get deeper to the living cells of the dermis, pH raises closer to neutral.
Note: the acid mantle theory has largely been disproven and is now used as an analogy only, as shown by the use of quotes in the medical literature. Despite what soap companies and outdated science may say, we don’t have an acidic film that we cleanse away. Instead, “acid mantle” is used only to denote the acidic nature of the skin surface.
Skin Barrier Function
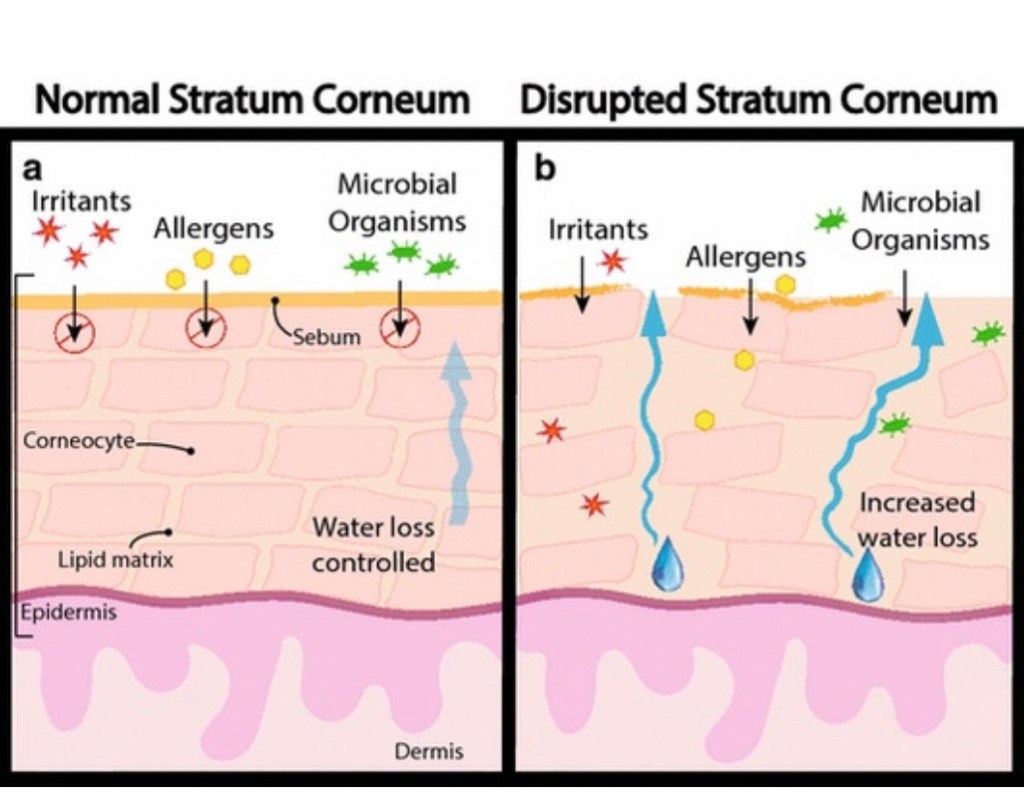
The role and function for the skin barrier encompasses quite a bit but can be primarily summarized as keeping moisture in and the bad stuff out. This includes allergens, irritants, and pathogens but also involves photoprotection against UV rays and neutralizing free radicals in addition to mounting an immune response. And of course, the skin protects us from mechanical damage like friction, scrapes, and impact.
Here is a great summary of some of the main functions of the stratum corneum:
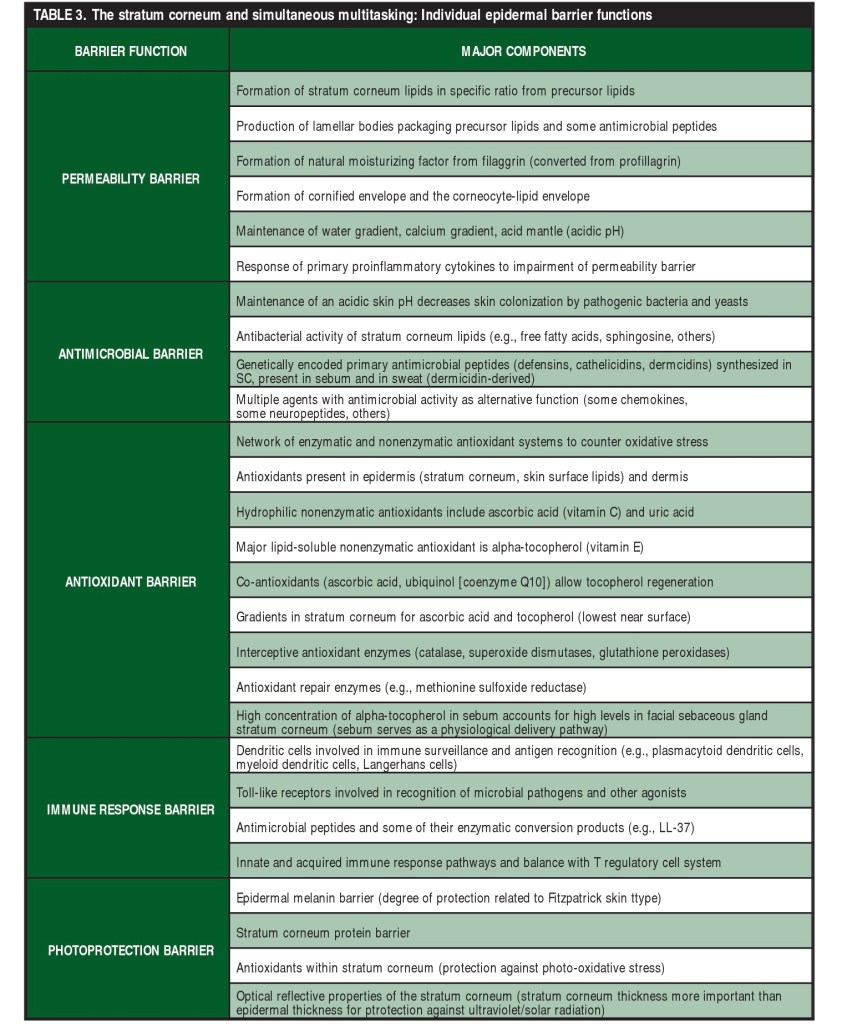
The Permeability Barrier
While the stratum corneum is technically dead, don’t let that fool you – that doesn’t mean it’s not biologically active. And hydration is critical to its flexibility as well as for the enzymes involved in desquamation (the shedding of dead skin cells).
20% of the body’s water can be found in the skin yet 60-70% of the skin’s water is found in the dermis alone. The epidermis isn’t vascular like the dermis and isn’t rehydrated via circulation so it relies diffusion from the dermis to obtain the necessary moisture and nutrients. Because the epidermis is the most superficial and exposed to our environment, a functioning skin barrier is essential to retaining moisture and minimizing trans epidermal water loss (TEWL).
We discussed the “brick and mortar skin model” above and how the bricks are the corneocytes differentiated from keratinocytes in the stratum granulosum while the lipids were also expressed from these skin cells. It’s worth mentioning though that the Natural Moisturizing Factor aka our skin’s humectants are housed within the corneocytes. Our endogenous amino acids, sodium PCA, urea, glycerin, and sodium lactate help attract and bind moisture.

Meanwhile, the lipids are mainly comprised of ceramides, cholesterol, and fatty acids and repel moisture unlike the corneocytes. If the skin barrier lipids are depleted or disorganized, the skin barrier cannot function properly. This can be due to the environmental factors like harsh cleansers as well as internal factors like inflammatory skin disorders which often disrupt the skin barrier lipids in particular. This can cause rough, dry skin and subsequently leads to dehydration as altered skin barrier function means water loss.
The humectants of the NMF also have important roles aside from drawing moisture from the environment. Products of degraded filaggrin, these humectants are responsible for the acidification of the skin surface and buffering capacity of the stratum corneum as well. So together with the skin barrier lipids, the corneocytes and their NMF are essential for everything from desquamation to wound healing, mediating inflammation, and barrier flexibility and homeostasis.
Other Barriers
As this is already summarized in the first image covering the functions of the stratum corneum, I won’t go into extensive detail here. But it’s important to remember that the skin barrier has multiple barrier facets and isn’t only about minimizing TEWL.
Something that wasn’t touched on above is that the stratum corneum has the highest concentration of internal antioxidants out of any layer of the skin. The antioxidant defenses of the stratum corneum are essential in neutralizing oxidative stress from the free radicals generated by environmental factors like UV radiation, visible light, and pollution. The antioxidant barrier is critical for protecting the skin against oxidative stress and DNA damage.
Meanwhile, there’s also an actual photoprotection barrier. While antioxidants neutralize free radicals once they’ve been generated, the skin also utilizes pigment forming cells like melanocytes to produce pigment. Melanin is one such example and can help block UV rays from entering the skin. It’s important to note though that regardless of how much natural protection your skin has, sunscreen is nonnegotiable.
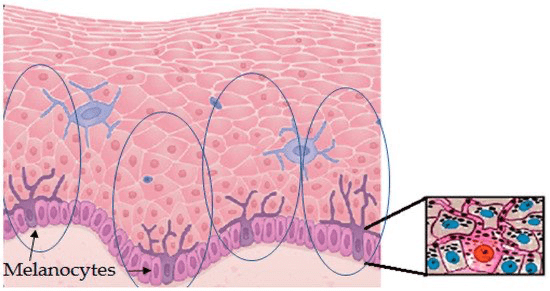
I’ll let you click the images above to research further on your own if you’re interested as far as the other barrier properties of the stratum corneum. But I do want to add that in regards to the antimicrobial barrier, we have antimicrobial peptides like defensins that help protect the skin against microbial invasion. Recent research has linked disruption of the antimicrobial defenses with skin disorders like atopic dermatitis.
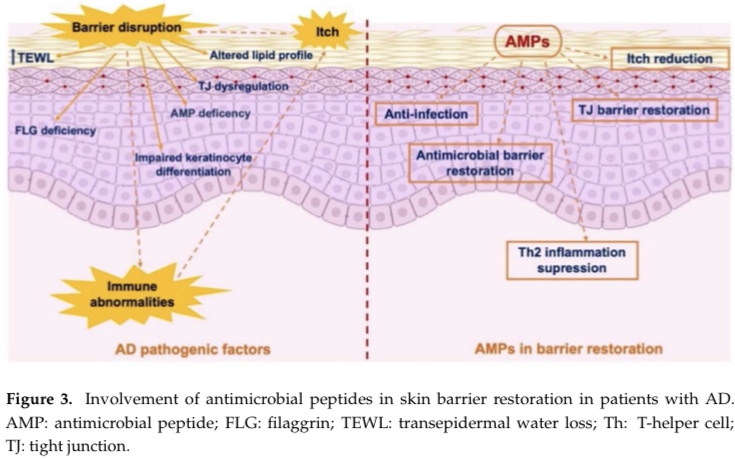
Impact of Altered Skin Barrier Function
We’ve covered the structure and function of the stratum corneum and its barrier functions as well as some of the short term repercussions of poor function. But I think it’s important to mention that it goes way beyond dehydration, desquamation, and xerosis (dry skin).
Alteration in skin barrier function is a common characteristic of acne prone skin, for example. It’s tricky to say whether impaired skin barrier is a contributor in acne or if acne is the cause since inflammatory skin disorders are known to disrupt skin barrier lipids. But we do know that acne patients have a higher skin surface pH, which will allow acne causing bacteria to thrive. Meanwhile, a return to normal barrier function will help with better desquamation, improved wound healing and inflammation, and a lower surface pH which means a less friendly environment to pathogenic microorganisms.
Acne isn’t the only skin disorder impaired by the function of the skin barrier and aside from skin disorders, its health is essential to protecting the skin from pathogens and other environmental factors as well. While not enough is known yet research wise on sensitive skin (since often symptoms are self reported), they have found that skin barrier impairment has been linked to sensitive and reactive skin types in preliminary research. This could be because compromised skin won’t adequately keep our allergens and irritants and decreased lipids have been observed in sensitive skin types for decades.
Skincare for Optimal Barrier Function
I don’t want anyone to automatically assume that their skin barrier function is compromised. Often I see anyone with normal to dry skin or even normal skin assume their skin barrier is somehow damaged.
It’s important to assess your skin and if you have very dry, sensitive, or over exfoliated skin or you’re someone with acne or another inflammatory skin disorder then you may benefit from skin barrier focused skincare. And anyone can benefit from the prevention suggestions I’ll cover.
Prevention:
- Use a gentle, low pH cleanser and don’t other cleanse
- Avoid harsh, stripping products like sulfates and alcohol based acne medications
- Practice moderation. Exfoliation and skin treatments that work via micro injury can be beneficial but give time to recovery as well so chronic inflammation and over exfoliation doesn’t result.
- If you have central heating or AC that’s very drying, consider a humidifier.
- Always use sunscreen and ideally an antioxidant serum as well to protect the skin barrier from environmental stressors
Skincare for Impaired Skin
- use products with barrier replenishing ingredients like ceramides, cholesterol, fatty acids, phytosterols, phytosphingosine, and lecithin
- also look for ingredients that help skin barrier function like niacinamide, urea (avoid if sensitive), n-acetyl glucosamine, panthenol, and allantoin
- anti inflammatory and wound healing ingredients like aloe vera, centella asiatica, bisbolol, growth factors, and snail mucin are great too
- hydration is absolutely key (especially beta glucan and hyaluronic acid) and using petrolatum over moisturizer will not only increase hydration but has been shown to diffuse into epidermal lipids and upregulate antimicrobial peptides for faster barrier recovery
- avoid anything irritating or that disrupts the skin barrier till fully recovered as well as common allergens and irritants like fragrance
See my Skin Barrier Rescue section of my Amazon store for specific products.
Skin Treatments (optional)
- Red light therapy
- Microcurrent, especially the microcurrent masks

As always, I hope this was helpful and educational for you all! Please comment below if you learned something new and what it was. Thank you for reading.
I highly recommend reading the previous deep dives on Skin Hydration and Free Radicals, Oxidative Stress, and Our Skin as they all really build off of each other. This post will also be really helpful in better understanding upcoming content in acne and other skin disorders, DNA Repair Enzymes, and skincare for deeper skin tones.
Don’t forget to shop my Amazon store and the section on Skin Barrier Rescue for my favorite products.
Leave a comment